“`html
H
A few days after their conversation, her daughter came to her, still grappling with the voices in her head. With her head down and tears in her eyes, she told her mother, “I want to understand what’s happening and get assistance.” Together, they took out their tablets and started searching for information on “What are hallucinations?”
Fact: If one twin in an identical pair has schizophrenia, the likelihood of the other twin developing it is 50%, regardless of their upbringing.
Years ago, I attended a session with a client and his psychiatrist. Barry was slouched in a chair, struggling to keep his eyes open as he shared how he hadn’t slept well recently.
When asked why, he ran his fingers through his hair and replied, “The voices have been intense.”
That was all she needed to hear.
Introduction
We’ve recently kicked off a three-part series focused on hallucinations, following a previous series that discussed dissociative experiences like derealization and depersonalization.
Our minds can conjure some bizarre scenarios, and it’s crucial to address these topics openly to gain understanding.
In the first part, we covered the basics of hallucinations. Now, we’ll explore the causes, including risk factors and triggers, and in the third part, we’ll discuss potential treatments.
Let’s dive in…
Understanding Hallucinations
Before we discuss causes, risk factors, and triggers, it’s important to cover the fundamentals found in part one.
Here’s a concise definition of a hallucination:
A hallucination occurs when a person perceives sensory experiences as real even though there is no actual external stimulus present.
As you may know, there are various types of hallucinations, with auditory hallucinations (mostly voices) being the most prevalent.
These experiences can stem from medication, illness, substance abuse, lack of sleep, and more. However, they are most commonly linked to schizophrenia and other psychotic disorders.
Causes: Risk Factors and Triggers
This can be frustrating. When we discuss the causes of mental and emotional illnesses, I wish I could provide clear-cut examples, similar to how one might explain diabetes. But since this isn’t achievable, we’ll focus on risk factors and triggers instead.
“For now, we’ll have to stick with risk factors and triggers while we figure this out.”
Fortunately, we can reference the diathesis-stress model, which suggests that mental disorders result from the interplay between a person’s latent vulnerability and external stressors.
Schizophrenia fits this model well. Research indicates a mix of genetic, physical, psychological, and environmental elements can heighten someone’s chances of developing the disorder.
Key Note
You might wonder why we’re discussing schizophrenia in an article primarily about hallucinations, given that numerous factors such as medications, certain illnesses, and more can produce them.
Here’s the truth: In psychiatric contexts, hallucinations linked to mental health disorders are the focus of research and treatment, unlike those caused by other medical conditions.
This is why schizophrenia is our main subject of discussion.
Risk Factors
Let’s begin identifying significant risk factors that could lead to a schizophrenia diagnosis…
Genetics
It’s well-known that schizophrenia often runs in families. This understanding comes from research involving identical twins, who share identical genetic material.
Fact: If one twin in an identical pair has schizophrenia, there is a 50% chance the other twin will also develop it, even if they were raised separately. Conversely, if one twin in a non-identical pair has the disorder, the other has a 13% chance of developing it.
Researchers still have much to learn about the genetics behind schizophrenia, but progress is being made.
For example, each human cell contains 23 pairs of chromosomes, which may undergo deletions or duplications. Recent findings indicate a small deletion in a specific part of chromosome 22 (referred to as 22q11) may be significant in a small fraction of schizophrenia cases, along with other serious health issues.
Interesting, isn’t it?
Brain Structure and Function
Let’s acknowledge a point that may seem obvious yet is often overlooked: emotional and mental health symptoms don’t just appear without reason. Brain structure and function play a crucial role.
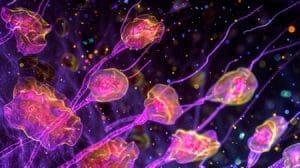
Electron microscopy showing the action of dopamine neurotransmitter receptors
Surprisingly, studies involving individuals with schizophrenia have identified subtle structural variations in their brains. While these differences may not appear in every individual diagnosed, and can also be present in those without any mental health issues, they are notable.
Most MRI studies regarding schizophrenia reveal consistently decreased volumes of gray matter in the medial temporal, superior temporal, and prefrontal regions of the brain.
Additionally, neurotransmitters, the chemicals responsible for transmitting messages between brain cells, are thought to be at atypical levels in individuals with schizophrenia, particularly dopamine.
The effectiveness of treatments that lower dopamine levels serves to support this theory.
Pregnancy and Birth Complications
Research indicates individuals who go on to develop schizophrenia often face complications before and during birth, such as:
- Low birth weight
- Premature birth
- Lack of oxygen (asphyxia)
- Exposure to infections
Such complications can lead to subtle…
“`
impact on cerebral growth.
Factors that Trigger Schizophrenia
Triggers represent a higher tier in the developmental spectrum. They are conditions that may lead to the onset of schizophrenia in individuals who are already at elevated risk. These include…
Stressful Situations
The primary psychological (environmental) factors that can trigger schizophrenia are overwhelming life changes, such as the loss of a loved one, unemployment, eviction, separation or divorce, and the end of a romantic relationship. Severe stress during childhood might also contribute to this.
Substance Abuse
Research indicates that drug use, especially cannabis, cocaine, LSD, or amphetamines, can heighten the chance of developing schizophrenia and other psychotic illnesses.
It remains uncertain whether drug use directly brings about symptoms in those who are vulnerable, or if a predisposition makes individuals more inclined to abuse substances.
Importantly, for anyone with a history of psychotic episodes, drug use can trigger a relapse or hinder treatment measures.
Additionally, studies have shown that adolescents and young adults who frequently use cannabis face a greater risk of developing schizophrenia as they age. This risk seems to increase with the use of more potent cannabis varieties. I’ve witnessed the unfortunate consequences in the E.R.
Why is it labeled a “mental disorder?”
Earlier, we explored the likelihood of developing schizophrenia from a genetic perspective. Interestingly, this risk can be likened to that of Alzheimer’s and Parkinson’s diseases. All three conditions share several characteristics.
So, why do we classify Alzheimer’s and Parkinson’s as neurodegenerative (neurological) diseases while categorizing schizophrenia as a mental disorder?
This distinction appears to be grounded in personal and societal effects. For Alzheimer’s and Parkinson’s, timely and effective care is usually accessible. In contrast, there are no such assurances with schizophrenia, leading to large numbers of individuals remaining untreated, homeless, or incarcerated.
Schizophrenia may genuinely warrant classification as a neurodegenerative (neurological) condition. However, due to its association with poorly understood suffering, impairment, intervention by law enforcement, and public health expenses, such reclassification has yet to take place.
Could stigma be a factor?
Anticipating Part Three
This wraps up our discussion on the causes: risk elements and triggers for hallucinations. Gaining knowledge is always the first step towards managing the situation. I hope this has been insightful.
Next, we will dive into our examination of treatments in part three. Stay tuned for that.
Once more, there’s a wealth of general information on hallucinations in part one. I encourage you to check it out.
I’d like to express my gratitude to Schizophrenia & Psychosis Action Alliance and the National Health Service for their valuable information support.
If you’re interested in more resources about emotional and mental health issues, take a look at the articles available on our page or browse by category below.

After struggling for decades with panic, generalized anxiety, mood swings, and alcohol dependency, Bill discovered his true calling: helping others facing similar challenges. At 49 years old, he pursued graduate studies and obtained his counseling credentials, continuing his work through Chipur and various initiatives.


